If you’re like most Mamas and planning to birth at hospital, there are a few things you need to know before you step foot through those doors.
Just as our bodies know how to make a baby and grow a baby, it knows how to birth a baby.
But don’t let this trick you into thinking everything will be fine if you just go with the flow.
Yes – your body is SO capable. But It also knows when NOT to birth a baby…
The environment you birth in needs to be similar to one that you’d be happy to ‘make a baby’ in…
There is no way you would be able to have sex if you were in fluorescent lighting, with several unfamiliar people watching, asking questions, touching you, offering interventions and drugs to help things along, machines and monitors surrounding you.
Bzzzt. Not going to happen.
So too, your body won’t birth a baby well in this environment… and although baby may still come out eventually, you’re certainly not likely to have a positive experience of it.
Cue birth trauma, postnatal depression, and hindered bonding and breastfeeding.
Birth is so crucial to the transformation of woman to mother.
Fortunately, there are lots of strategies you can use to give yourself the best chance of a more positive and less painful birth experience.
So here are five of the ways hospital could make labour more painful, and how you can overcome them.

1. They can block the labour hormones.
THE ISSUE: Hospital environments can completely block the labour hormones you need to minimise your pain, make your labour easier, and promote normal physiology of birth.
Bright lights, being talked at, unfamiliarity with people and environment – these all block oxytocin and endorphins, and increase adrenaline.
That means you’re more likely to have stalled/slow labour, more likely to need drugs and interventions (which come with their own gamut of risks and issues), and more likely to feel fearful and out of control.
The stress hormone adrenaline also affects baby, and can increase bleeding in women.
Simply put, if you don’t feel private, safe and unobserved in labour, your incredible birthing hormones won’t work to their full potential to minimise your pain and help labour progress smoothly.
THE SOLUTION: Research & apply it! Watch ‘positive birth videos’ on Youtube to see how ‘doable’ birth can be.
Learn about your natural pain-relieving hormones in labour and how to boost those hormones. Dr Sarah Buckley is the guru of this. You can find her resources here.
Make a list of tools that you and your support people can use to help you through labour and birth. Dads and partners are great at setting the environment up!
You can learn what tools will be beneficial through Hypnobirthing Australia, Lamaze Childbirth Education, and for Dads only – Beer + Bubs.
If you’re looking for affirmation cards for birth, caesarean, or Dads/Partners/support people, check out our shop.
If you can, find a ‘continuity of care’ Midwife or Private Midwife, the experts in physiological birth.
They will care for you throughout your pregnancy and birth, get to know you, protect your space, and advocate for your wishes.
If interventions are required for your or your baby’s safety, they will ensure you are fully informed and your physical and emotional well being are protected.

2. They monitor ‘progress’ meticulously, yet can also stall it.
THE ISSUE: By the text books, a woman should have three contractions every ten minutes in labour and a baby can be born when a cervix is fully dilated (10 centimetres).
These factors in a hospital setting are often used as end-goals.
The end goal is to maintain labour at a rate of three contractions every ten minutes, and to get to fully dilated, progressing at a rate of 0.5cm an hour of a first time mum or 1cm an hour for a woman having her second or more child.
Like our bodies are well oiled machines that have to perform efficiently to a linear timeline.
The reality is, babies don’t read text books, and labour and birth is not linear – it is not a numbers game.
I’ve witnessed women birth babies with ‘only’ two irregular contractions every ten minutes. I’ve witnessed women get to fully dilated and have difficulty birthing because of the way their baby is positioned.
There is so much more to the physiology of childbirth than the numbers.
Evidence shows when we expect birth to be linear and place these unrealistic goals and numbers on labour, women are more likely to have unnecessary interventions.
Interventions, which pose risks to mothers a babies. Women are more likely to have continuous monitoring strapped to their bellies.
More likely to have many vaginal examinations. More likely to have drugs, which can slow labour.
And more likely to have synthetic hormones (which block your natural hormones) to augment the labour progression…. all leading to increased adrenaline and increased perception of pain.
All of these factors hinder the physiological processes that are needed for labour and birth to occur.
Then we wonder why labour hasn’t ‘progressed’, and often, the women are the ones left feeling like a failure, when really it is the maternity system that has let them down.
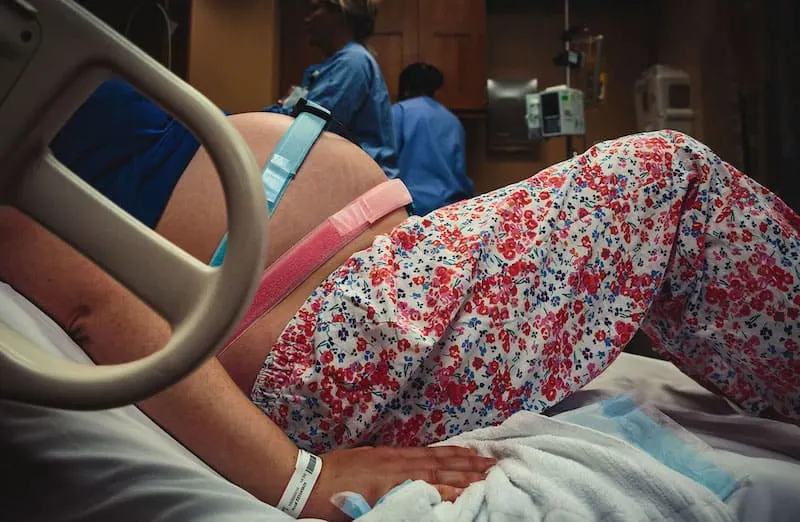
THE SOLUTION: Learn about the stages of labour, and what the signs are of each stage. It is common, particularly for first time mothers, to have a latent phase prior to establishing labour.
Latent labour can stop and start, sometimes fizzling out all together and not starting again for days or another week.
To avoid the progression of labour being affected by disruption to your hormones and physiology, if safe to do so, remain home during latent/early labour, and move in to hospital when you are confident and showing signs of established labour.
There are lots of tools you can use at home in for comfort in latent phase which you can find here.
Once you do move in to the hospital, it is important to have a care provider who understands the physiology of birth, how positioning of babe can affect labour/birth and how to overcome this, external signs of progress such as behaviours, ‘the purple line’, bloody show, fetal ejection reflex etc., and when intervention is necessary or unnecessary. We explore this more in point 4.
3. Unnecessary interventions are more likely to occur.
THE ISSUE: As we discussed in point 2, for many reasons, the hospital environment can contribute to increasing your risk of unnecessary interventions, leaving you vulnerable to the risks associated with them and the ‘cascade of interventions’.
When interventions are utilised, birth is more painful, because your pain relieving and coping hormones can’t do their work.
But how can we know whether a procedure or intervention being offered/recommended is in fact necessary or the safest option?

THE SOLUTION: Get educated about all things birth! Not just physiological birth, but birth variations and complexities too.
Tip – you will have to look outside generic antenatal classes for this information.
Some great resources to find the evidence surrounding interventions are Evidence Based Birth and Dr Rachel Reed’s articles at MidwifeThinking.
When you are being advised of a procedure or intervention, remember your right to informed consent.
Informed consent means consent that has been received having discussed all benefits, risks and options with a woman.
One may consent to something, but if they haven’t been given the opportunity to discuss all of these factors it doesn’t count.
The best way to ensure you receive all the information you need to give informed consent is to use the BRAIN acronym in discussions and asking questions of health care providers.
B – What are the benefits (of the procedure)?
R – What are all the risks involved?
A – What are the alternatives?
I – What does your intuition tell you?
N – What if we do nothing? OR Not right now, we’d like some time to discuss it.
By using these strategies, you’re giving yourself the best chance at only having intervention if it’s appropriate, and therefore you’re more likely to feel in control of your birth, safe, supported, and (magical hormones) less pain!
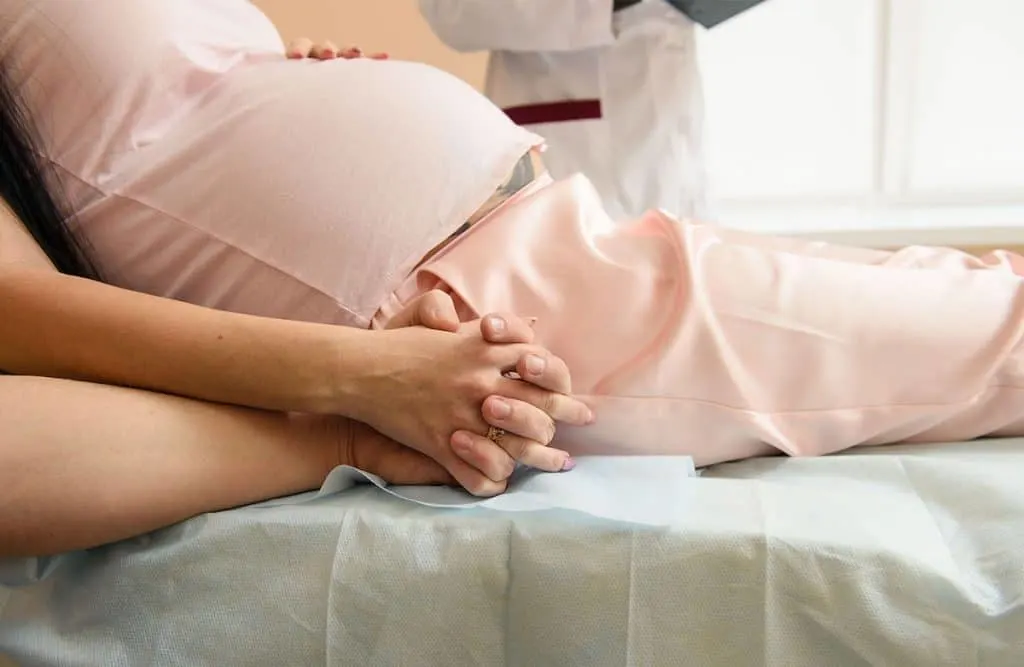
4. They are unfamiliar with you & you are unfamiliar with them.
THE ISSUE: It’s most likely that when you arrive to a hospital birth suite in labour, you don’t know them, and they don’t know you.
Statistics show that only 8% of women in Australia have access to a ‘continuity of Midwifery carer’ model, which is also known to be the gold standard of maternity care as it promotes best outcomes for Mamas and babes.
The issue here is that trying to labour when you are surrounded by strangers is really hard!
Your flight or fight response kicks in and that adrenaline takes over, so too, does your heightened perception of pain.
The other part of this is that your care provider on the day won’t have an intimate knowledge of you as an individual person, your history, your wishes surrounding birth, what’s important to you as a woman, mother, family.
Therefore they can’t provide you with personalised care.
THE SOLUTION: Seek out a continuity of Midwifery carer model of care. In Australia, this is a Private Midwife, where you will have your own Midwife care for you in pregnancy, labour/birth and 6 weeks postnatally.
The other option in Australia is to be cared for by a Midwifery Group Practice (MGP), where you may have one Midwife or a small team of Midwives from pregnancy through to the postnatal period.
A Private Midwife is an independent practitioner who can care for you in the hospital and outside of the hospital, while MGP Midwives are employees of the hospital.
The evidence shows women who access continuity of Midwifery carer are more likely to have a physiological ‘normal’ birth.
Continuity of care Midwives are the experts in physiological birth.
Because they are the experts, they are also very in tune to when labour and birth is falling outside of ‘normal’ and they know how to get you the appropriate care/interventions when required.
If you do not have access to a Private Midwife or MGP Midwife in your area, it is so important to have a birth plan in place.
A birth plan outlines your birth preferences, not only in the situation of everything ‘going to plan’, but also in the event of complications.
The value of a birth plan isn’t in the plan itself, it’s in the process of becoming informed.

5. They can be constricting of your movement and comfort.
THE ISSUE: Walk into any Birth Suite, and the crisp white starched bed will be the centre focus of the room. Next to the monitoring equipment that often requires you to lay down.
With a long cultural history of viewing birth as a medical event that sometimes happens naturally, rather than a natural event that sometimes needs medical help, it’s not surprising most women instinctively walk in and head straight to lay down on the bed.
It’s what they think is expected of them.
Sometimes, women are even asked to be on the bed, on their backs, for the convenience of the caregiver.
There is so much you need to know about why restricted movement and labouring on your back is not beneficial to an easier birth, and makes it more painful.
Luckily, I’ve already written about it here.
THE SOLUTION: Find out whether your hospital has equipment/facilities that promote an active, upright birth – gym balls, shower, bath, floor mats, birth stools.
If not… first ask ‘why not?’, and take in whatever you can from home.
And lastly, start practicing upright positions you might like to use in labour during pregnancy.
This will give you a good idea of what feels good and what doesn’t.
Don’t forget to include your birth partner! Juju Sundin’s book, Birth Skills, is a great resource for learning about active, upright birth strategies.
Another resource that has great affect on easier pregnancy, labour and birth is Spinning Babies.
Happy birthing! You’ve got this.






















